What Is Scleroderma and Who Is a Good Candidate for Treatment?
What Is Scleroderma?
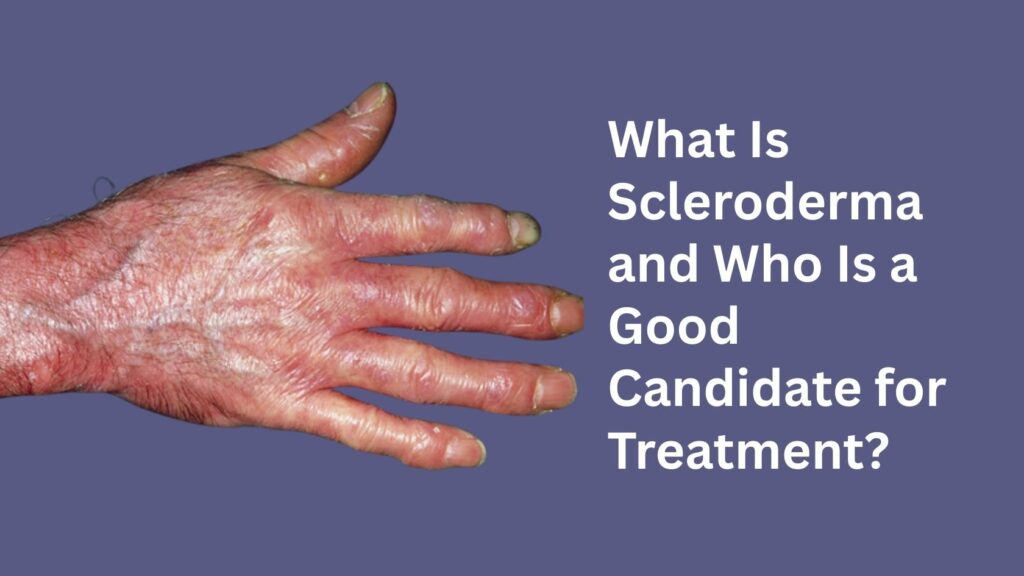
Scleroderma is a chronic autoimmune condition that affects the skin and connective tissues. The term “scleroderma” means “hard skin,” referring to one of its most noticeable symptoms—skin thickening and tightening. However, scleroderma is more than a skin condition. It can also affect blood vessels, joints, muscles, and internal organs such as the lungs, heart, kidneys, and digestive system.
Scleroderma develops when the immune system becomes overactive and stimulates excessive collagen production. Collagen is a protein that provides structure to skin and tissues. When too much collagen accumulates, tissues become thickened, stiff, and sometimes damaged.
Understanding what scleroderma is and recognizing who may benefit from treatment helps ensure early diagnosis, proper care planning, and improved long-term outcomes.
Types of Scleroderma
Scleroderma is broadly categorized into two main types:
1. Localized Scleroderma
Localized scleroderma primarily affects the skin and sometimes underlying tissues such as muscle. It does not typically involve internal organs. It may appear as patches of hardened skin or linear streaks on the body.
Although localized scleroderma can cause cosmetic and mobility concerns, it is generally less severe than systemic forms.
2. Systemic Scleroderma (Systemic Sclerosis)
Systemic scleroderma affects not only the skin but also internal organs. It is further classified into:
Limited systemic scleroderma – Usually progresses slowly and often affects the skin of the hands, arms, and face.
Diffuse systemic scleroderma – Can progress more rapidly and may involve larger skin areas and internal organs.
Systemic involvement requires careful monitoring and long-term management.
Common Symptoms of Scleroderma
Symptoms vary depending on the type and severity of the condition.
Skin Symptoms
Thickened, tight, or shiny skin
Reduced flexibility in fingers
Hard patches on skin
Changes in skin pigmentation
Circulation Symptoms (Raynaud’s Phenomenon)
Fingers or toes turning white, blue, or red in response to cold or stress
Numbness or tingling
Painful episodes
Joint and Muscle Symptoms
Joint stiffness
Swelling
Muscle weakness
Reduced range of motion
Digestive Symptoms
Acid reflux
Difficulty swallowing
Bloating
Constipation
Lung and Heart Symptoms
Shortness of breath
Persistent dry cough
Fatigue
Irregular heartbeat in some cases
Kidney Involvement
Elevated blood pressure
Swelling
Changes in urine output
Early symptom recognition is important because scleroderma may affect multiple body systems.
What Causes Scleroderma?
The exact cause of scleroderma is not fully understood. However, several factors are believed to contribute:
Autoimmune system dysfunction
Genetic predisposition
Environmental triggers
Abnormal collagen production
It is not contagious and does not spread from person to person.
How Is Scleroderma Diagnosed?
Diagnosis involves a combination of:
Detailed medical history
Physical examination
Blood tests (autoantibodies and inflammation markers)
Imaging tests
Lung and heart function tests
Skin evaluation
Because symptoms may overlap with other autoimmune diseases, accurate diagnosis is essential before starting treatment.
Who Is a Good Candidate for Scleroderma Treatment?
Scleroderma treatment is not one-size-fits-all. The decision to begin treatment depends on symptoms, severity, organ involvement, and overall health status.
Below are individuals who are generally considered good candidates for treatment.
1. Individuals with Progressive Skin Thickening
Patients experiencing increasing skin tightness, reduced flexibility, or spreading hardened patches are strong candidates for treatment. Early intervention may help slow progression and preserve mobility.
2. Patients with Raynaud’s Phenomenon and Circulation Problems
Those experiencing frequent circulation attacks, finger ulcers, or severe color changes in fingers and toes benefit from treatment aimed at improving blood flow and preventing complications.
3. Individuals with Internal Organ Involvement
Patients with lung, heart, kidney, or digestive system involvement require structured medical management. Treatment may help protect organ function and reduce long-term complications.
4. People with Joint Pain and Reduced Mobility
Persistent joint stiffness, swelling, or muscle weakness affecting daily function indicates the need for treatment and supportive therapies.
5. Patients Experiencing Respiratory Symptoms
Shortness of breath or persistent cough may indicate lung involvement. Early evaluation and treatment help slow progression and maintain lung capacity.
6. Individuals with Digestive Complications
Patients with severe reflux, swallowing difficulties, or malabsorption issues benefit from targeted treatment to improve comfort and nutrition.
7. Patients with Elevated Blood Pressure Related to Scleroderma
Kidney involvement requires prompt medical attention. Individuals showing signs of high blood pressure or kidney stress are candidates for immediate evaluation and treatment.
8. Individuals Seeking Early Intervention
Even patients with mild symptoms may benefit from early treatment. Early intervention often reduces the risk of long-term complications.
Goals of Scleroderma Treatment
Treatment focuses on:
Controlling immune system activity
Slowing collagen buildup
Improving blood circulation
Reducing inflammation
Protecting internal organs
Managing pain and stiffness
Preventing complications
Preserving independence and quality of life
Because scleroderma can be chronic, long-term monitoring is often required.
Treatment Options for Scleroderma
Treatment varies based on symptoms and organ involvement.
Immunosuppressive Therapy
Helps reduce immune overactivity and slow disease progression.
Circulation-Improving Medications
Used to manage Raynaud’s phenomenon and prevent ulcers.
Lung-Specific Therapy
Helps protect lung function in patients with interstitial lung disease or pulmonary hypertension.
Digestive System Management
Includes reflux control and nutritional support.
Kidney Protection
Regular blood pressure monitoring and kidney function checks.
Physical Therapy
Maintains joint mobility and muscle strength.
Skin Care Support
Prevents dryness, cracking, and infection.
Treatment plans are customized and adjusted over time.
Importance of Monitoring
Monitoring plays a key role in scleroderma care. Regular follow-up helps detect changes early.
Monitoring may include:
Blood pressure checks
Lung function testing
Heart evaluations
Kidney function tests
Skin assessments
Medication safety monitoring
Early detection of complications improves outcomes.
When to Seek Immediate Medical Attention
Urgent evaluation is required if a patient experiences:
Sudden severe breathlessness
Rapid swelling
Severe headaches with high blood pressure
Chest pain
Painful finger ulcers
Sudden kidney-related symptoms
Prompt treatment reduces serious risks.
Living with Scleroderma
Living with scleroderma involves ongoing care, symptom awareness, and lifestyle adjustments. Many individuals maintain productive lives with proper management.
Helpful strategies include:
Protecting hands from cold
Staying physically active within comfort limits
Managing stress
Following medication schedules
Attending regular follow-up visits
Consistency and education improve long-term stability.
Final Overview
Scleroderma is a complex autoimmune condition that affects skin, blood vessels, and internal organs. Understanding the disease and identifying who is a good candidate for treatment supports timely intervention and improved outcomes.
Good candidates for treatment include individuals with progressive symptoms, circulation problems, organ involvement, joint stiffness, digestive complications, or early warning signs. Early diagnosis and structured care planning are essential in managing scleroderma effectively.
With personalized treatment, careful monitoring, and supportive lifestyle strategies, many individuals are able to control symptoms and maintain independence over time.
Frequently Asked Questions
1. What is scleroderma?
Scleroderma is a chronic autoimmune condition that causes skin thickening and may affect blood vessels, joints, muscles, and internal organs.
2. What is the difference between localized and systemic scleroderma?
Localized scleroderma mainly affects the skin, while systemic scleroderma can involve internal organs such as the lungs, heart, kidneys, and digestive system.
3. Who is a good candidate for scleroderma treatment?
Individuals experiencing progressive skin tightening, circulation problems, joint stiffness, or internal organ involvement are good candidates for treatment.
4. Can mild scleroderma symptoms require treatment?
Yes, early treatment may help slow disease progression and prevent complications even if symptoms are mild.
5. What are the early signs of scleroderma?
Early signs may include Raynaud’s phenomenon, skin tightening, joint stiffness, swelling, acid reflux, and fatigue.
6. Is scleroderma a curable condition?
There is currently no cure for scleroderma, but treatment can help manage symptoms and protect organ function.
7. Does scleroderma affect internal organs?
Yes, systemic scleroderma may affect organs such as the lungs, heart, kidneys, and digestive tract.
8. How is scleroderma diagnosed?
Diagnosis involves medical history, physical examination, blood tests, and organ function assessments.
9. Why is monitoring important in scleroderma treatment?
Regular monitoring helps detect organ involvement early, track disease progression, and adjust treatment safely.
10. When should someone seek immediate medical attention for scleroderma?
Immediate medical care is needed for sudden breathlessness, chest pain, severe high blood pressure, new kidney symptoms, or painful finger ulcers.

Dr. Binoy J. Paul
MD, PhD, DNB, FRCP (Edin.)
Senior Consultant Rheumatologist