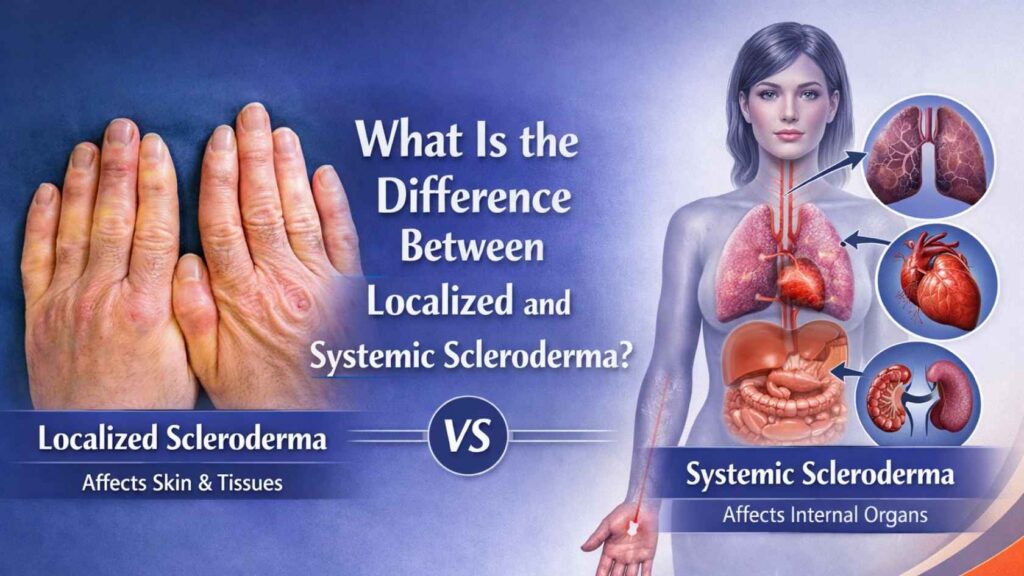
What Is the Difference Between Localized and Systemic Scleroderma?
Scleroderma is a chronic autoimmune condition that causes hardening and tightening of the skin due to excessive collagen production. However, not all forms of scleroderma are the same. The condition is broadly divided into two main categories: localized scleroderma and systemic scleroderma (also known as systemic sclerosis). Understanding the difference between these two forms is important because their symptoms, progression, and health impact vary significantly.
Both localized and systemic scleroderma involve abnormal immune system activity and collagen buildup, but they represent two distinct clinical conditions.
What Is Localized Scleroderma?
Localized scleroderma primarily affects the skin and sometimes the tissues just beneath it. It may also involve underlying fat or muscle in certain cases. However, it usually does not affect major internal organs.
Localized scleroderma often appears as:
Hardened patches of skin (morphea)
Linear streaks or bands on limbs or face
Skin discoloration or thickening
In most cases, localized scleroderma remains limited to specific areas of the body and does not spread to internal systems. It may improve over time, especially with appropriate care.
What Is Systemic Scleroderma?
Systemic scleroderma affects not only the skin but also the blood vessels and internal organs. It is considered more serious because it can involve:
Lungs
Heart
Kidneys
Digestive system
Unlike localized scleroderma, systemic scleroderma may impact overall body function and can become life-threatening if major organs are affected.
It often includes:
Widespread skin tightening
Circulation problems
Fatigue
Joint stiffness
Digestive issues
Organ-related complications
Systemic scleroderma typically requires long-term monitoring and structured treatment.
Key Differences Between Localized and Systemic Scleroderma
1. Organ Involvement
Localized Scleroderma:
Affects only the skin and underlying tissues such as fat or muscle. Internal organs are usually not involved.Systemic Scleroderma:
Affects the skin as well as internal organs like the lungs, heart, kidneys, and gastrointestinal tract.
2. Raynaud’s Phenomenon
Localized Scleroderma:
Raynaud’s phenomenon is uncommon.Systemic Scleroderma:
Raynaud’s phenomenon is often an early and common sign. It causes fingers or toes to change color in response to cold or stress.
3. Disease Progression
Localized Scleroderma:
Usually remains confined to specific skin areas and rarely progresses to systemic disease. In some cases, it may improve over time.Systemic Scleroderma:
Often progressive and may worsen without proper management.
4. Symptoms and Severity
Localized Scleroderma:
Causes skin plaques, bands, or tightening without major systemic symptoms.Systemic Scleroderma:
Can cause widespread skin changes along with fatigue, joint pain, digestive issues, breathing problems, and potential organ complications.
5. Age Group Affected
Localized Scleroderma:
More commonly seen in children and adolescents.Systemic Scleroderma:
More frequently diagnosed in adults between 30 and 50 years of age.
6. Types
Localized Scleroderma Includes:
Morphea (patch-like thickening)
Linear scleroderma (band-like changes)
Systemic Scleroderma Includes:
Limited systemic sclerosis
Diffuse systemic sclerosis
These subtypes help determine disease behavior and management needs.
Similarities Between the Two Forms
Despite their differences, both localized and systemic scleroderma share some common features:
Both are autoimmune conditions
Both involve excessive collagen production
Both are chronic in nature
Both may require long-term monitoring
Both can affect quality of life
However, the extent of impact differs significantly.
Why This Difference Matters
Understanding whether a person has localized or systemic scleroderma is essential because:
Treatment plans differ
Monitoring requirements vary
Prognosis is different
Risk of complications is not the same
Localized scleroderma is generally less severe, while systemic scleroderma may require comprehensive care due to potential organ involvement.
Summary
Localized scleroderma mainly affects the skin and nearby tissues and rarely involves internal organs. Systemic scleroderma affects the skin, blood vessels, and major organs such as the lungs, heart, or kidneys, making it more complex and potentially serious.
Although both conditions share autoimmune origins and collagen overproduction, they represent two distinct clinical diseases with different progression patterns and health implications. Recognizing the difference helps guide diagnosis, treatment planning, and long-term monitoring.
Frequently Asked Questions
1. What is localized scleroderma?
Localized scleroderma mainly affects the skin and sometimes the underlying tissues such as fat or muscle, without involving major internal organs.
2. What is systemic scleroderma?
Systemic scleroderma affects the skin, blood vessels, and internal organs like the lungs, heart, kidneys, and digestive system.
3. Does localized scleroderma affect internal organs?
No, localized scleroderma usually does not involve internal organs.
4. Can systemic scleroderma become life-threatening?
Yes, systemic scleroderma can become serious if major organs are affected.
5. Is Raynaud’s phenomenon common in both types?
Raynaud’s phenomenon is rare in localized scleroderma but common in systemic scleroderma.
6. Do both types progress in the same way?
No, localized scleroderma often remains stable or improves, while systemic scleroderma may progress over time.
7. Which type is more common in children?
Localized scleroderma is more commonly seen in children.
8. Which type is more common in adults?
Systemic scleroderma is more frequently diagnosed in adults between 30–50 years.
9. Are both types autoimmune conditions?
Yes, both localized and systemic scleroderma are autoimmune conditions involving excessive collagen production.
10. Do both require long-term monitoring?
Yes, although systemic scleroderma requires more extensive monitoring due to possible organ involvement.
BAARC Rheumatology Specialists

Dr Athul Paul
MD, Post Doctoral Fellowship in Rheumatology (CMC Vellore)
Consultant Rheumatologist
BAARC Rheumatology Clinic, Kozhikode

Dr Binoy J Paul
MD, PhD, DNB, FRCP (Edin.)
Senior Consultant Rheumatologist
BAARC Rheumatology Centre, Kozhikode