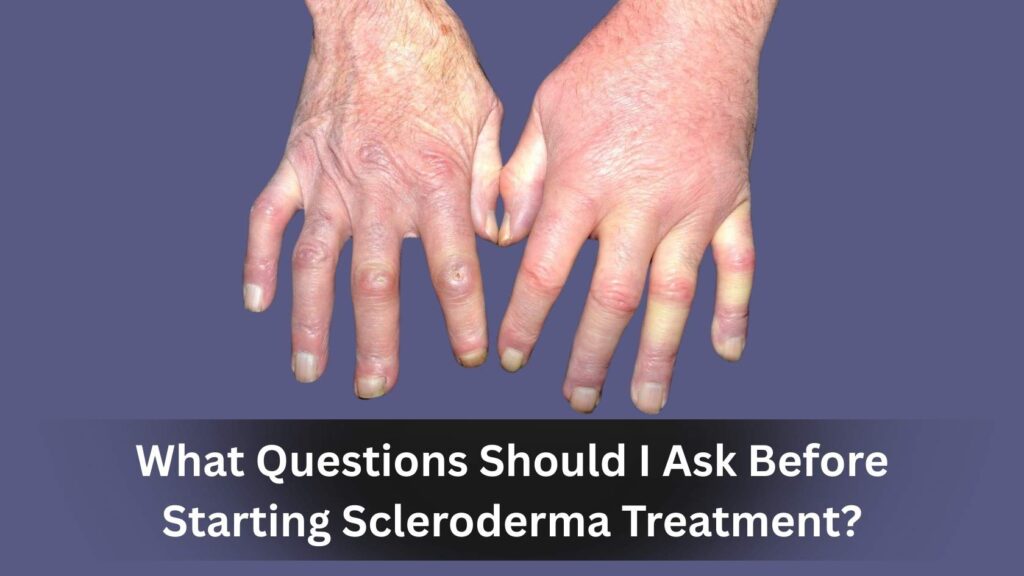
What Questions Should I Ask Before Starting Scleroderma Treatment?
Starting treatment for scleroderma is an important step that requires clear understanding, careful planning, and active patient involvement. Scleroderma is a chronic autoimmune condition that can affect the skin, blood vessels, joints, digestive system, lungs, heart, and kidneys. Because treatment often involves long-term monitoring and individualized care plans, asking the right questions before beginning therapy helps ensure better outcomes and improved confidence.
This guide outlines the essential questions you should ask before starting scleroderma treatment and explains why each topic matters.
1. What Type of Scleroderma Do I Have?
Scleroderma is not a single condition. It may be:
Localized scleroderma (mainly affecting the skin)
Limited systemic scleroderma
Diffuse systemic scleroderma
Understanding the exact type helps determine:
Disease progression risk
Organ involvement
Treatment intensity
Monitoring frequency
Clarifying your diagnosis is the first and most important step.
2. Which Organs Are Affected?
Scleroderma can involve internal organs such as:
Lungs
Heart
Kidneys
Digestive tract
Ask your healthcare provider:
Have my lungs been evaluated?
Is my heart functioning normally?
Are my kidneys affected?
Do I need additional organ tests?
Knowing which systems are involved helps tailor your treatment plan.
3. What Are the Goals of My Treatment?
Scleroderma treatment goals vary depending on disease stage and severity.
You should ask:
Is the goal to reduce inflammation?
Are we aiming to slow skin thickening?
Is organ protection the priority?
What improvements can I expect?
Clear goals help set realistic expectations and track progress effectively.
4. How Long Will Treatment Last?
Scleroderma treatment is often long-term.
Important questions include:
Is this a short-term treatment or ongoing plan?
How often will my treatment be reviewed?
When will we evaluate progress?
Understanding duration prepares you mentally and practically for continuous care.
5. What Medications Will I Need?
Treatment may include:
Immunosuppressive medications
Circulation-improving therapy
Lung-protective medications
Digestive symptom management
Blood pressure control
Ask:
Why is this medication recommended?
How does it work?
How long will I need it?
Medication clarity improves adherence and safety.
6. What Are the Possible Side Effects?
All treatments may carry risks.
Ask:
What are common side effects?
What warning signs should I watch for?
When should I seek urgent medical care?
Will I need regular blood tests?
Understanding risks helps prevent complications.
7. How Will My Condition Be Monitored?
Monitoring is essential in scleroderma treatment.
Ask:
How often will I need lung tests?
Will my heart be evaluated regularly?
How will kidney function be monitored?
How often should blood pressure be checked?
Regular monitoring ensures early detection of changes.
8. How Will Treatment Affect My Daily Life?
Scleroderma treatment may impact work, exercise, and daily activities.
Ask:
Can I continue my normal routine?
Are there activity restrictions?
Should I modify my diet?
How can I protect my skin and joints?
Knowing lifestyle adjustments helps prevent flare-ups.
9. What Should I Do If Symptoms Worsen?
Flare-ups may occur even during treatment.
Ask:
What signs indicate worsening disease?
When should I schedule an urgent visit?
Can flare-ups be managed at home?
Clear instructions improve safety and reduce anxiety.
10. How Can I Support My Treatment with Lifestyle Changes?
Lifestyle habits influence treatment success.
Ask about:
Safe exercise routines
Skin protection strategies
Raynaud’s management
Stress reduction techniques
Nutrition recommendations
Active participation improves long-term stability.
11. What Are the Long-Term Expectations?
Scleroderma is often chronic.
You should ask:
What is my long-term outlook?
Can symptoms stabilize?
What complications should I watch for?
How can progression be minimized?
Understanding expectations builds realistic planning.
12. Are There Any Tests I Should Complete Before Starting Treatment?
Before beginning therapy, baseline assessments may include:
Blood tests
Lung function testing
Heart evaluations
Kidney function checks
Ask whether additional testing is necessary for safe treatment initiation.
13. Will I Need Physical Therapy?
Joint stiffness and reduced mobility are common.
Ask:
Should I start physical therapy now?
What exercises are safe?
How often should I practice mobility exercises?
Early therapy helps preserve movement.
14. How Will My Blood Pressure Be Managed?
Kidney involvement may cause high blood pressure.
Ask:
Should I monitor blood pressure at home?
What readings require immediate attention?
Proper monitoring prevents serious complications.
15. What Emotional Support Resources Are Available?
Chronic illness may affect mental health.
Ask:
Are educational materials available?
How can I manage stress?
Are support groups recommended?
Emotional preparation supports long-term care.
16. What Happens If Treatment Does Not Work?
Not all patients respond the same way.
Ask:
What are alternative treatment options?
When would adjustments be made?
How will we evaluate effectiveness?
Knowing backup plans reduces uncertainty.
17. How Often Should Follow-Up Visits Be Scheduled?
Follow-up frequency depends on disease activity.
Ask:
How soon is my next appointment?
What tests will be repeated?
How often will monitoring occur?
Structured follow-up prevents complications.
18. Can Early Treatment Improve Outcomes?
Early intervention is often beneficial.
Ask:
Has my condition been detected early?
How does early treatment affect prognosis?
Timely treatment can slow progression and protect organs.
Importance of Asking Questions
Open communication builds trust and improves treatment success. Patients who ask informed questions are more likely to:
Follow medication schedules
Attend follow-up visits
Recognize warning signs
Maintain consistent lifestyle adjustments
Being proactive enhances safety and long-term disease control.
Summary
Before starting scleroderma treatment, it is essential to ask detailed questions about your diagnosis, organ involvement, treatment goals, medication options, monitoring plans, side effects, lifestyle adjustments, and long-term expectations. Because scleroderma is a complex autoimmune condition, clear communication ensures personalized care and safer long-term management.
Preparation, awareness, and active participation in treatment decisions can significantly improve health outcomes and quality of life.
Frequently Asked Questions
1. Why is it important to ask questions before starting scleroderma treatment?
Asking questions helps you understand your diagnosis, treatment goals, possible risks, and long-term care plan, allowing you to make informed decisions.
2. What should I know about my specific type of scleroderma?
You should understand whether you have localized, limited systemic, or diffuse systemic scleroderma, as treatment and monitoring differ for each type.
3. Should I ask about organ involvement before treatment?
Yes, it is important to know if your lungs, heart, kidneys, or digestive system are affected so that treatment can be properly planned.
4. What questions should I ask about medications?
Ask why the medication is prescribed, how it works, how long you will need it, and what side effects to monitor.
5. Is it necessary to discuss possible side effects?
Yes, understanding potential side effects helps you recognize warning signs early and seek medical attention when needed.
6. How often should monitoring tests be done?
Monitoring frequency depends on disease severity and organ involvement, but regular follow-up tests are essential for safe management.
7. Can lifestyle changes support my treatment?
Yes, gentle exercise, skin protection, stress management, and avoiding smoking can help improve treatment outcomes.
8. Should I ask about long-term expectations?
Yes, understanding the long-term outlook helps you set realistic goals and prepare for ongoing care.
9. What should I do if my symptoms worsen during treatment?
You should ask your healthcare provider about warning signs, emergency symptoms, and when to schedule urgent evaluation.
10. Can early treatment improve outcomes?
Yes, early diagnosis and timely treatment often help slow progression and reduce complications.

Dr. Binoy J. Paul
MD, PhD, DNB, FRCP (Edin.)
Senior Consultant Rheumatologist